Our newest paper has just been published in the Journal of Refractive Surgery (available here – open access). In it we have examined the effects a procedure called corneal crosslinking has on the structure of the cornea, on the chemical bonds within it and how those relate to changes to the stiffness (strength) of the tissue. This crosslinking procedure is a standard treatment for the common corneal condition Keratoconus. The findings we haver repored are interesting from a bio-physics standpoint but, importantly, we think they will also be useful reference standards against which future improvements to therapies for keratoconus can be tested.
 This work was led by Shao-Hsuan Chang a multi-disciplinary PhD student jointly supervised between Profs Ahmed Elsheikh (Engineering at University of Liverpool), Colin Willoughby (Corneal surgeon, now at the University of Ulster) and Kevin Hamill (Matrix biology at the University of Liverpool).
This work was led by Shao-Hsuan Chang a multi-disciplinary PhD student jointly supervised between Profs Ahmed Elsheikh (Engineering at University of Liverpool), Colin Willoughby (Corneal surgeon, now at the University of Ulster) and Kevin Hamill (Matrix biology at the University of Liverpool).
This page will describe the project in quite general terms, however, the paper is available online now and is open access you can read it here.
Keratoconus
Keratoconus is a progressive eye disease in which the normally round cornea thins and begins to bulge out into a cone-like shape. This cone shape deflects light in an aberrant way as it enters the eye, this means the lights hits the retina in wrong and this leads to distorted vision.  This disorder affects approximately 1 in 450 people, usually being diagnosed in teens/young adults.
This disorder affects approximately 1 in 450 people, usually being diagnosed in teens/young adults.
Although keratoconus itself does not cause blindness, it does lead to severely impaired vision. Importantly this visual impairment gets worse and worse as the patient ages. The corneal bulging continues to grow as the corneal structure is weak and constantly under pressure from the fluid within the eye. Ultimately, it is only through transplant that normal vision can be restored (read more about the condition and efforts toward better treatments here and about the lab visit last year of paralympic athlete Stephanie Slater who has keratoconus here).
Corneal transplant is not without risk and currently there is a worldwide shortage of donor corneas available (so tell your family that you are willing to donate your eyes to allow others to see after you die!). Therefore treatments focus on slowing the worsening of the disorder and that’s where corneal crosslinking (CXL) comes in.
Corneal crosslinking
CXL involves scraping away the epithelial layer of the cornea (painful!!) then dosing the corneal stroma with riboflavin (a photoactivator) and exposing the soaked cornea to UV light to, in theory, crosslink the proteins and proteoglycans in the stroma. These crosslinks are thought to improve the strength of the cornea and thereby prevent further growth of the cone. The procedure has been used clinically in Europe for a number of years now and has relatively recently been approved for use in the US. However, surprisingly little is known about how exactly it works and, because of this, most of the improvements to the protocol have come about from trial and error-type approaches.
Shao’s project has therefore tried to address this problem by generating a set of benchmark measurements in terms of the biomechanical changes induced by the “standard” CXL treatment protocol. Having these benchmarks in place is important; it is against these that future improvements and new ways to cross-link corneas without using UV can be compared.

The resulting work “Determination of the relationship between mechanical properties, ultrastructural changes and intrafibrillar bond formation in corneal UVA/riboflavin cross-linking treatment for keratoconus” has just been published in the Journal of Refractive Surgery (link).
In this paper, Shao performed a series of mechanical, chemical and biological tests on corneas treated with each of the individual parts of the CXL protocol individually and together in order to build up a picture of what each contributes to the overall therapeutic effect.
Results
On each pair of eyes Shao determined how they responded in terms of changes to thickness and stiffening. The results revealed that the dextran solution that the riboflavin was dissolved in caused dehydration of the tissue, but once you accounted for that there was no further change in corneal thickness. However, UVA-mediated crosslinking caused a ~25% increase in stiffness compared with corneas treated with just dextran.
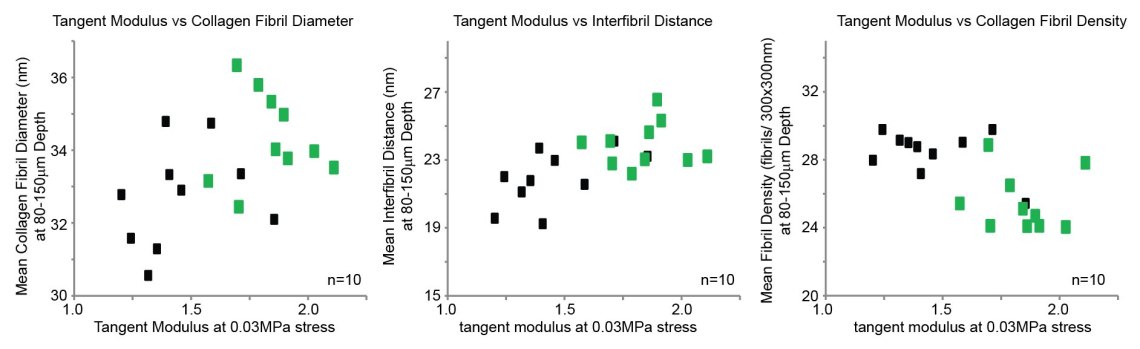
Shao also used electron microscopy (generating some beautiful images) to investigate what happens at the structural level to the collagen fibrils within the cornea. These were done on the same eye so we could directly compare the results. These data revealed that comparing the full treatment to dextran only, there were increases in collagen fibril diameter and decreases in number of fibrils per unit area but only in the uppermost 250μm of the treated tissues.


Finally Shao also looked at what happened at the intra-fibrillar bond level, using a procedure termed Fourier-transform infrared spectroscopy (wiki link). This revealed an increase in C-O stretch and conversion rats of amide bonds. This supports a model where the procedure creates new intrafibril bonds.
Most studies of this type investigate either the mechanics or the biology or the biochemistry of a procedure, it’s relatively rare to get all three done in one experimental system. By performing both the mechanical and the ultrastructural analyses on the same eye, the data allow us to infer how the measured changes to collagen structures within the cornea influence the stiffness characteristics. Importantly, our results confirm that none of these individual aspects is able to give you the full picture without also knowing about the others.
What does this all mean together…. probably best explained with a picture!
Our working model
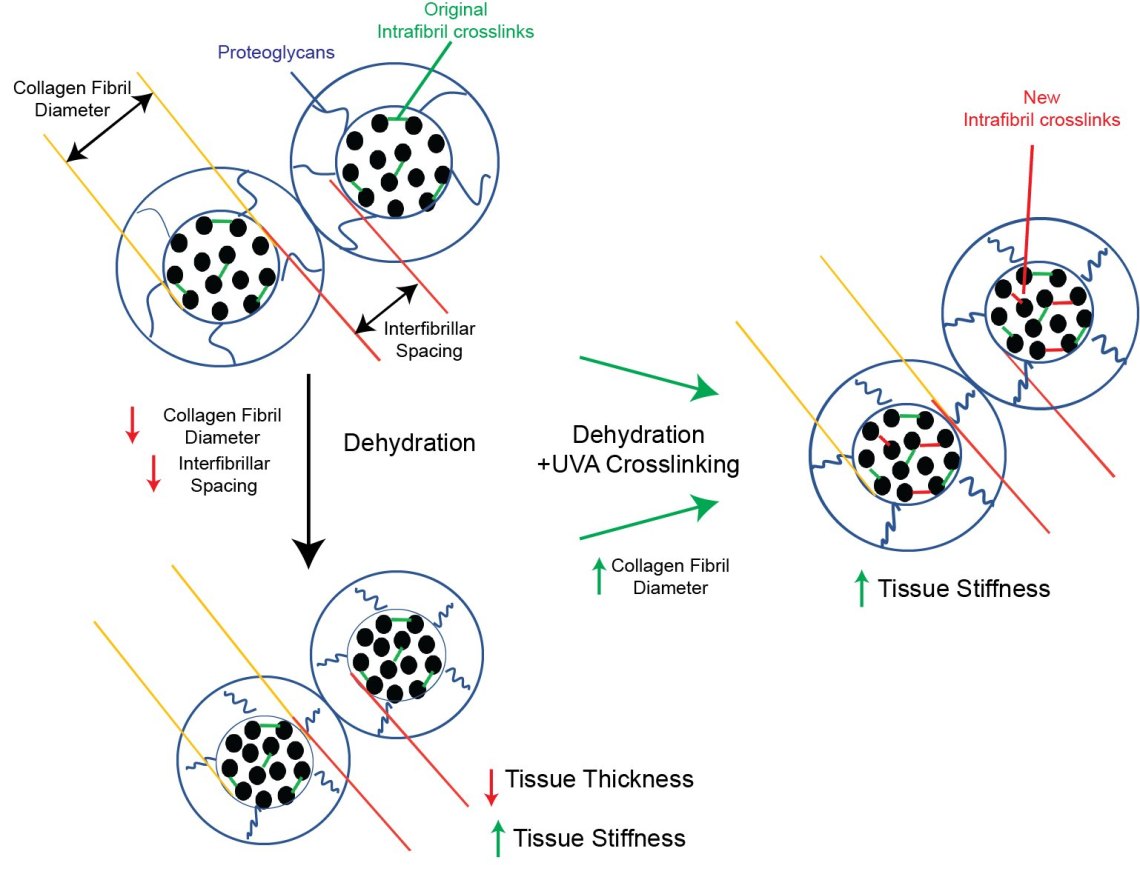
This work is a really interesting for me to be involved in. the interplay between the mechanics and the biology is really important to fully understanding how structures “work” and what goes wrong. Although, as a biologist, it’s been a steep learning curve to try to get my head around what exactly was being measured and what the data means! This has also been a really valuable experience that will influence other projects that are ongoing in the lab.
Shao has worked hard to generate the data in this paper and we really hope that it will be a useful resource for others in CXL field, and therefore help future developments and improvements to treat keratoconus.
Please share widely, the paper is open access so should be free to all.
You can read the final paper here
More about keratoconus here
About the Hamill lab and other projects here or via the menu above.
If you want to donate to eye research, I recommend the charity Fight For Sight, they support work at all levels from discovery science right through to the clinic.



